Hematopoietic Stem/Progenitor Cells
Hematopoietic Stem Cells (HSC) are cells isolated primarily from bone marrow and umbilical cord blood. They can self-renew and differentiate into many different types of blood cells [1] (Figure 1).
These characteristics raised the interest of researchers in using them as potential cellular treatment for a variety of diseases over 50 years ago. Nowadays, transplant of HSC is routinely used as therapy for several cancers, blood or immune disorders and metabolic diseases[2], [3]. Moreover, research progress could widen the therapeutic window of HSC transplants to treat brain disorders such as Alzheimer or Dementia, or neurodegenerative diseases such as Multiple Sclerosis, amongst others[2]–[8].
In vitro challenges
In vitro cultures of HSC still represent a challenge in research because their fragility prevents them from replicating and also because, in order to differentiate, samples of HSC must be cultured with a highly specific combination of cytokines[9], [10]. Additionally, given their similarity to many other blood or bone marrow cells, purifying HSC is a challenge, and the fact that only 1:10000-15000 bone marrow cells or 1:100000 blood cells is known to be a stem cell[1] does not ease the task. To address the identification problem, cell surface protein markers [11] can be used. One of the most commonly used markers for HSC recognition is CD34, a transmembrane phosphoglycoprotein encoded by the gene with the same name[12]. CD34+ HSC isolated from umbilical cord blood present the advantage to efficiently proliferate without losing their ability to differentiate into the several blood cell types[13].
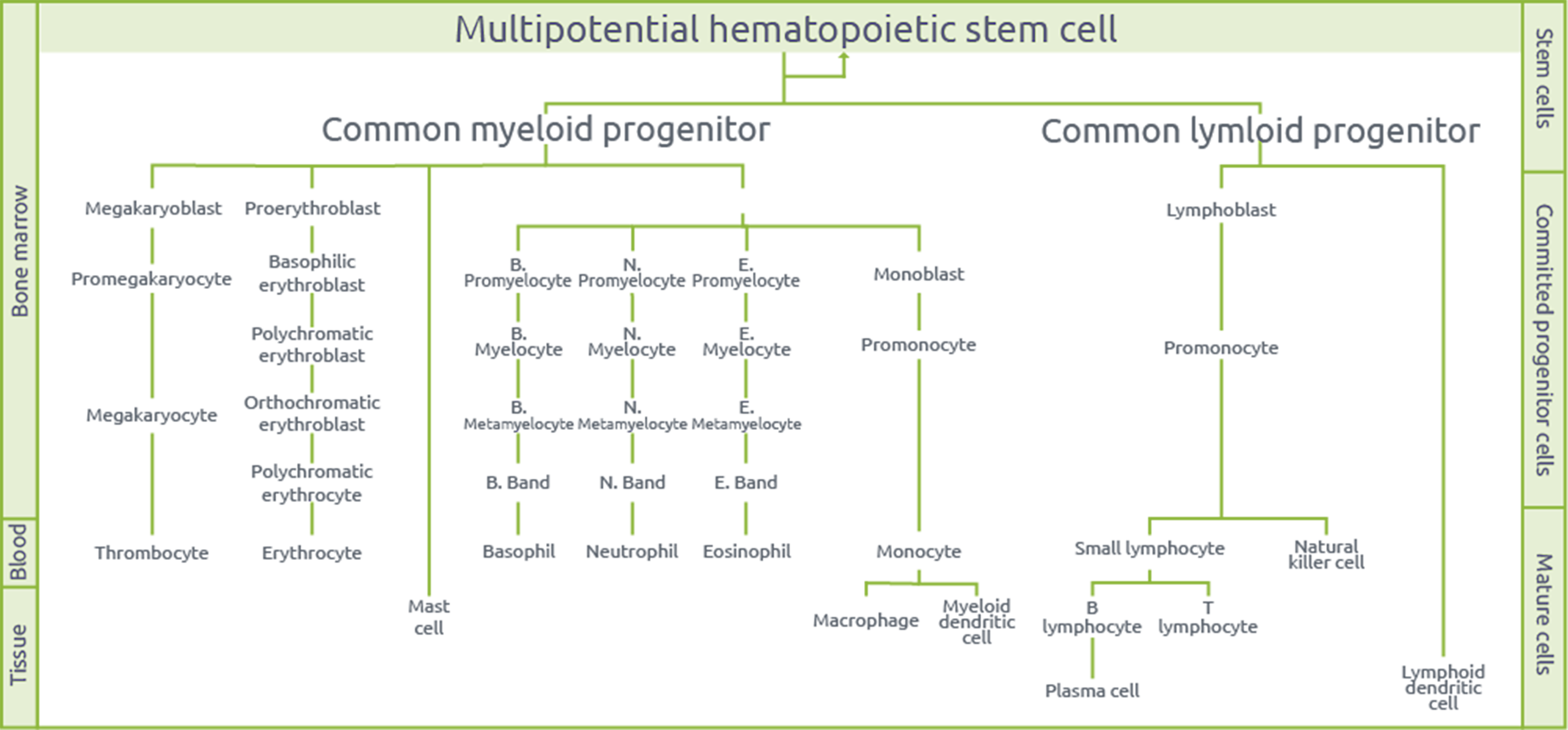
Figure 1. Multipotency of hematopoietic stem cells.
Observation of a mitosis in an umbilical cord blood isolated CD34+ HSC sample
A sample of human cord blood CD34+ stem/progenitor cells kindly provided by Lonza was cultured in X-VIVOTM 15 serum-free hematopoietic cell medium, supplemented with recombinant human thrombopoietin (25ng/mL), Rlt3 ligand (25ng/mL) and stem cell factor (13ng/mL). The culture was also coated with fibronectin.
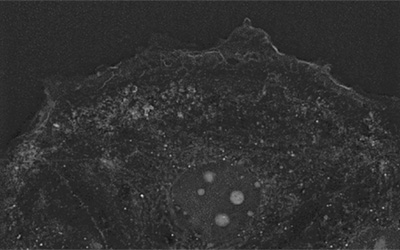
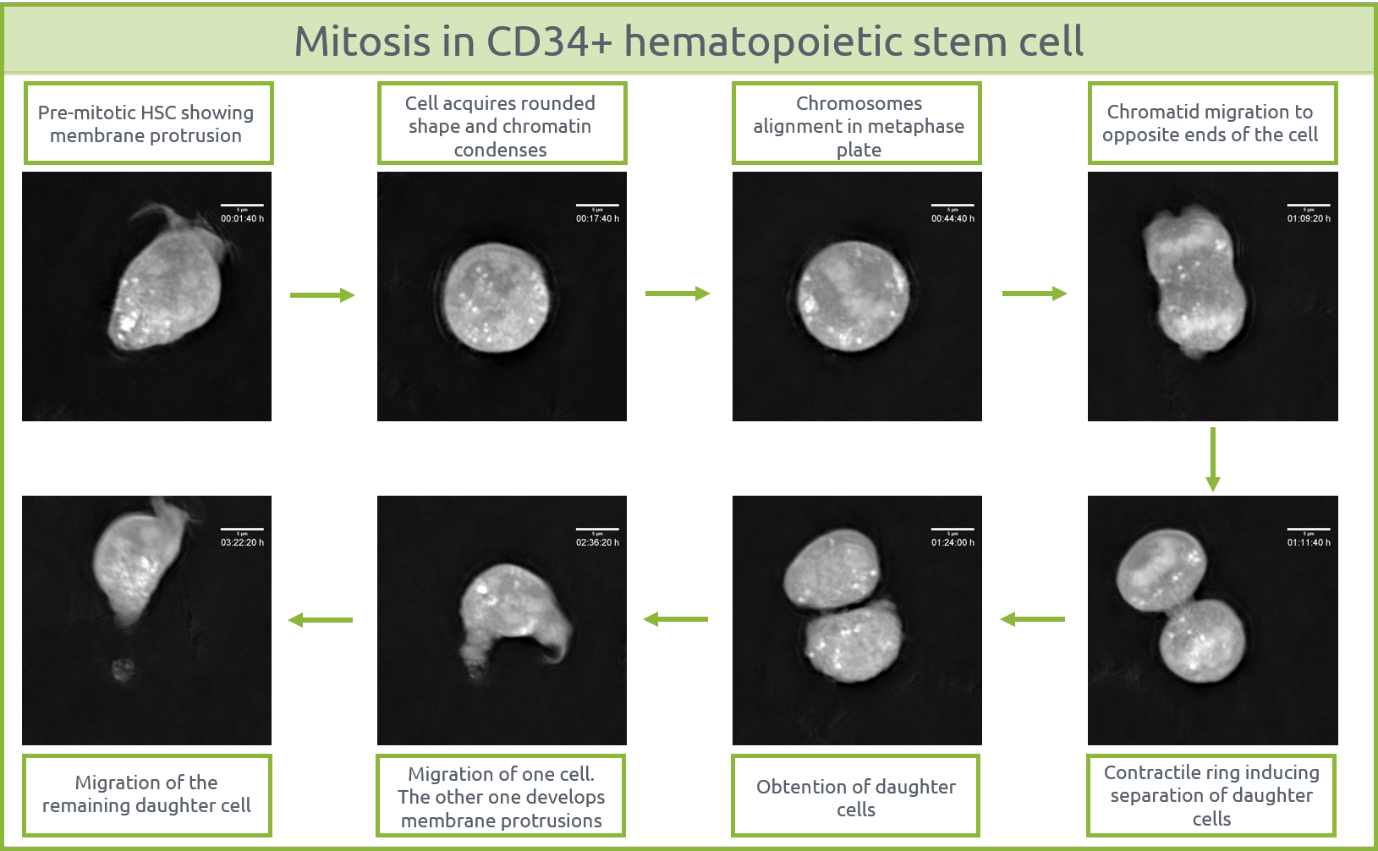
A remarkably long live cell observation (3 images/min during 15hours) was performed with Nanolive’s 3D Cell Explorer, and a cell division was captured. To date and to our knowledge, this live cell movie featuring CD34+ HSC is the first one ever obtained.
One can distinguish characteristic steps of mitosis such as chromatin condensation inside the nucleus that lead to chromosome formation, the alignment of the chromosomes in the metaphase plate and the migration of sister chromatids to opposite ends of the cells. Eventually, two daughter cells were obtained as a result of the contractile ring effect during cytokinesis (Figure 2).
Considering that any stress would trigger programmed cell death in such a sensitive cell type, the mitosis captured acquires further significance. Indeed, it is a sign of not just the homogeneity of the cell culture, but also of the fact that both the medium and freezing procedures of the sample were optimal and that Nanolive’s technology was completely non-invasive, which can also be reaffirmed by observing healthy behavior in most of the cells surrounding the dividing cell.
[1] “5. Hematopoietic Stem Cells | stemcells.nih.gov.” [Online]. Available: https://stemcells.nih.gov/info/2001report/chapter5.htm.
[2] “Hematopoietic Stem Cells: What Diseases Can these Stem Cells Treat?” [Online]. Available: https://bioinformant.com/what-diseases-are-treatable-with-hematopoietic-stem-cells-hsc-from-cord-blood/.
[3] Y. M. Hawsawi, F. Al-Zahrani, C. H. Mavromatis, M. A. Baghdadi, S. Saggu, and A. A. A. Oyouni, “Stem Cell Applications for Treatment of Cancer and Autoimmune Diseases: Its Promises, Obstacles, and Future Perspectives.,” Technol. Cancer Res. Treat., vol. 17, p. 1533033818806910, 2018.
[4] A. Tyndall and J. M. van Laar, “Stem cells in the treatment of inflammatory arthritis,” Best Pract. Res. Clin. Rheumatol., vol. 24, no. 4, pp. 565–574, Aug. 2010.
[5] T. Franceschetti and C. De Bari, “The potential role of adult stem cells in the management of the rheumatic diseases,” Ther. Adv. Musculoskelet. Dis., vol. 9, no. 7, p. 165, 2017.
[6] C. A. Rush, H. L. Atkins, and M. S. Freedman, “Autologous Hematopoietic Stem Cell Transplantation in the Treatment of Multiple Sclerosis,” Cold Spring Harb. Perspect. Med., vol. 9, no. 3, p. a029082, Mar. 2019.
[7] G. I. Fouad, “Stem cells as a promising therapeutic approach for Alzheimer’s disease: a review,” Bull. Natl. Res. Cent., vol. 43, no. 1, p. 52, Dec. 2019.
[8] S. Rivest, “S1-03-03: Hematopoietic stem cells as a cure for Alzheimer’s disease,” Alzheimer’s Dement., vol. 4, no. 4, p. T103, Jul. 2008.
[9] S. J. Morrison, D. E. Wright, S. H. Cheshier, and I. L. Weissman, “Hematopoietic stem cells: challenges to expectations,” Curr. Opin. Immunol., vol. 9, no. 2, pp. 216–221, Apr. 1997.
[10] M. A. Walasek and OffPage), Hematopoietic stem cell expansion. s.n.], 2012.
[11] I. L. Weissman and J. A. Shizuru, “The origins of the identification and isolation of hematopoietic stem cells, and their capability to induce donor-specific transplantation tolerance and treat autoimmune diseases.,” Blood, vol. 112, no. 9, pp. 3543–53, Nov. 2008.
[12] D. L. Simmons, A. B. Satterthwaite, D. G. Tenen, and B. Seed, “Molecular cloning of a cDNA encoding CD34, a sialomucin of human hematopoietic stem cells.,” J. Immunol., vol. 148, no. 1, pp. 267–71, Jan. 1992.
[13] D. K. Kim, Y. Fujiki, T. Fukushima, H. Ema, A. Shibuya, and H. Nakauchi, “Comparison of hematopoietic activities of human bone marrow and umbilical cord blood CD34 positive and negative cells.,” Stem Cells, vol. 17, no. 5, pp. 286–94, 1999.
Read our latest news
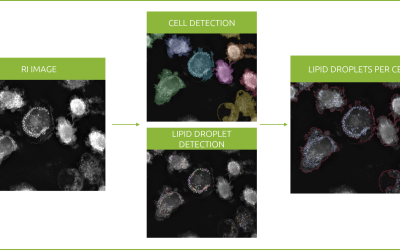
Revolutionizing lipid droplet analysis: insights from Nanolive’s Smart Lipid Droplet Assay Application Note
Introducing the Smart Lipid Droplet Assay: A breakthrough in label-free lipid droplet analysis Discover the power of Nanolive's Smart Lipid Droplet Assay (SLDA), the first smart digital assay to provide a push-button solution for analyzing lipid droplet dynamics,...
Food additives and gut health: new research from the University of Sydney
The team of Professor Wojciech Chrzanowski in the Sydney Pharmacy School at the University of Sydney have published their findings on the toxic effect of titanium nanoparticles found in food. The paper “Impact of nano-titanium dioxide extracted from food products on...
2023 scientific publications roundup
2023 has been a record year for clients using the Nanolive system in their scientific publications. The number of peer-reviewed publications has continued to increase, and there has been a real growth in groups publishing pre-prints to give a preview of their work....
Nanolive microscopes

3D CELL EXPLORER
Budget-friendly, easy-to-use, compact solution for high quality non-invasive 4D live cell imaging

3D CELL EXPLORER-fluo
Multimodal Complete Solution: combine high quality non-invasive 4D live cell imaging with fluorescence

CX-A
Automated live cell imaging: a unique walk-away solution for long-term live cell imaging of single cells and cell populations